Solutionreach Unveils First Ever Revenue Cycle Messaging™ Solution Learn More
Digital Patient Intake Management
Help your patients arrive prepared
Automatically send HIPAA-compliant digital forms that patients can fill out anytime, anywhere.

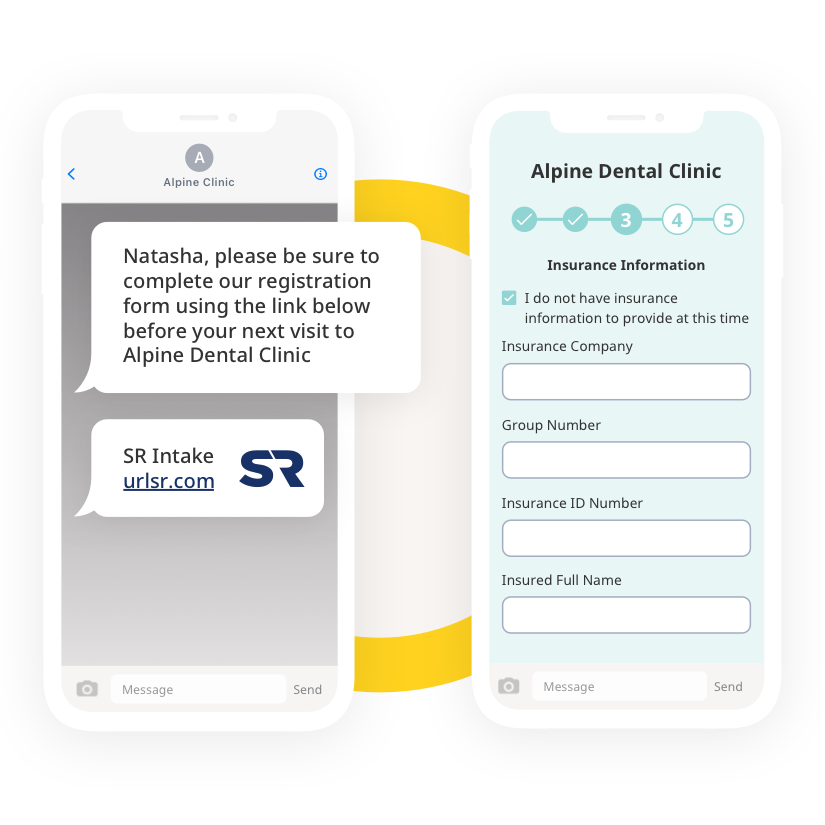
Intake forms killing your flow? We can help.
Paper intake, apps, and even sign-in portals can cause check-in delays and waiting room pileups. Switch to digital intake with Solutionreach to streamline patient intake management for everyone.
- Customize intake forms for your practice
- Automatically send to new patients via email or text message
- Write-back demographic data to your PM or EHR*
*Automatic write-back available on select practice management systems
